When people hear terms like vascular disease or vision disease, it is easy to assume they all mean the same thing. Add diabetes into the mix, and things get even more confusing. One of the most common questions patients ask is whether retinal vascular disease and diabetic retinopathy are the same condition.
Short answer: no. They are related, but they are not identical. Understanding the difference matters because early diagnosis and treatment can prevent serious vision damage.

Let’s break it down in plain language.
What Is Diabetic Retinopathy?
Diabetic retinopathy is a specific eye condition caused by diabetes. Over time, high blood sugar damages the tiny blood vessels in the retina, the light-sensitive tissue at the back of the eye responsible for vision. When those vessels weaken, leak, or become blocked, retinal issues begin.
In early stages, diabetic retinopathy may not cause noticeable symptoms. As it progresses, patients may experience blurry vision, floaters, dark spots, or even sudden vision changes. Left untreated, it can lead to permanent vision damage.
Because it directly results from diabetes blood pressure fluctuations and high glucose levels, this condition is closely tied to how well a person manages their overall health.
That is why an annual diabetic vision exam and routine eye test diabetes screenings are critical.
What Is Retinal Vascular Disease?
Retinal vascular disease is a broader category. It refers to any condition that affects the blood vessels in the retina. Diabetes is one cause, but not the only one.
Other causes include:
- High blood pressure
- Blood clots
- Inflammatory conditions
- Age-related vascular changes
For example, retinal vein occlusion and retinal artery occlusion are forms of vascular disease that can occur even in people without diabetes.
So here is the key distinction: diabetic retinopathy is a type of retinal vascular disease, but not all retinal vascular disease is diabetic retinopathy.
Think of it like squares and rectangles. Every square is a rectangle, but not every rectangle is a square.
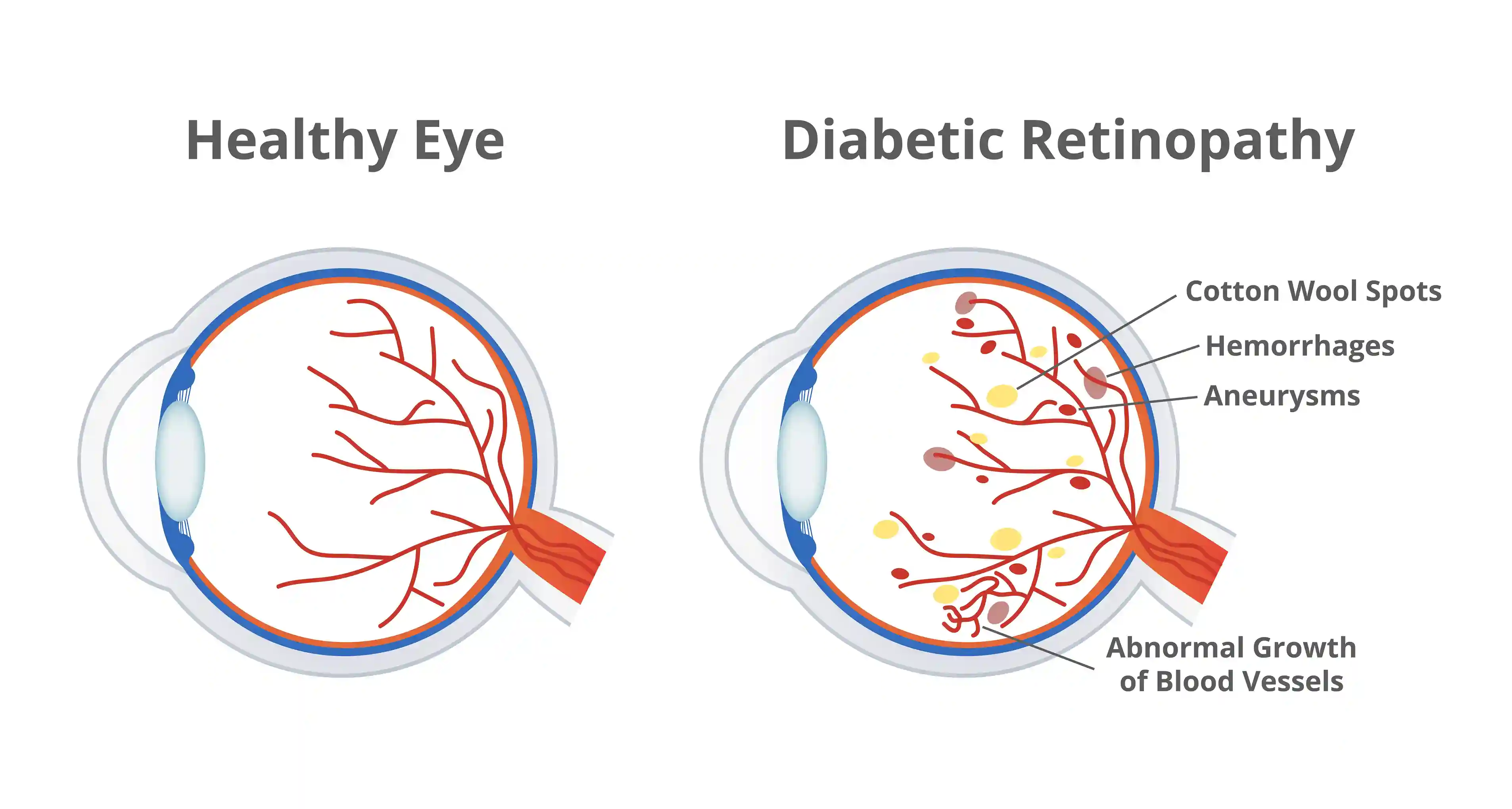
How Diabetes and Blood Pressure Affect the Retina
The retina depends on a delicate network of blood vessels to function properly. When diabetes blood pressure levels are uncontrolled, those vessels undergo stress. High blood sugar damages vessel walls, while high blood pressure increases strain on already fragile structures.
Over time, this leads to leakage, swelling, or abnormal new vessel growth. This process is what defines diabetic retinopathy and explains why managing systemic health is just as important as eye care.
Ignoring these warning signs increases the risk of long-term vision disease and irreversible vision damage.
Symptoms: Are They Different?
Symptoms can overlap significantly because both conditions affect retinal blood vessels.
Common warning signs include:
- Blurred or fluctuating vision
- Dark or empty areas in vision
- Floaters
- Distorted vision
- Sudden vision loss
In diabetic retinopathy, symptoms often develop gradually. In other forms of retinal vascular disease, such as a vein occlusion, vision changes may occur suddenly.
That difference in speed can sometimes help guide diagnosis and treatment decisions.
How a Retina Specialist Makes the Diagnosis
A retina specialist uses advanced imaging to evaluate the blood vessels and retinal tissue. During a diabetic vision exam or comprehensive eye test diabetes evaluation, the doctor may perform:
- Dilated eye examination
- Optical coherence tomography (OCT)
- Fluorescein angiography
- Retinal photography
These tests help identify swelling, bleeding, blocked vessels, or abnormal new vessel growth. Accurate diagnosis and treatment depend on identifying the root cause of the vascular problem.
This is not something you want guessed at. The retina is delicate, and early detection changes outcomes dramatically.
Diabetic Retinopathy Treatment vs Other Vascular Treatments
Treatment depends on the severity and underlying cause.
Diabetic retinopathy treatment may include:
- Anti-VEGF injections to reduce swelling and abnormal vessel growth
- Laser therapy
- Vitrectomy surgery in advanced cases
For other types of retinal vascular disease, treatment may also involve injections or laser therapy, but managing blood pressure, clotting disorders, or systemic inflammation becomes a bigger part of the strategy.
The overlap exists, but the long-term management plan can differ significantly.
Why Early Screening Matters
Here is the uncomfortable truth: many patients with diabetic retinopathy feel fine until significant damage has already occurred. Vision disease can progress silently.
That is why consistent diabetic vision exam appointments are non-negotiable for anyone with diabetes. Even if vision seems normal, the retina may already show early vascular changes.
Catching problems early allows for timely diabetic retinopathy treatment and reduces the risk of severe vision damage.
Waiting for symptoms is like waiting for smoke before checking if something is burning.
So, Are They the Same?
No. Retinal vascular disease is the umbrella term. Diabetic retinopathy is one specific condition under that umbrella caused by diabetes.
Understanding the difference is more than semantics. It shapes how doctors approach diagnosis and treatment, and it reinforces why systemic health management plays such a powerful role in protecting vision.
If you have diabetes blood pressure concerns, fluctuating blood sugar, or unexplained vision changes, seeing a retina specialist is not optional. It is a preventative strategy.
Vision is remarkably resilient, but it is not indestructible. The retina’s blood vessels are tiny, precise structures. When they are stressed repeatedly, the damage accumulates quietly.
Smart patients do not wait for vision damage to become obvious. They treat routine screening like maintenance for something irreplaceable, because it is.
